By Margaret Evans
It was late August 2012. In Crawford County, Pennsylvania, Jessie Woodworth was eager to get home from work. She and her daughter, Loretta, had planned an evening ride. At home her husband, Bob, had checked the horses in their sixty acre pasture. Little Bit, their big Foundation Quarter Horse, was near the gate. But he could see no sign of their six-year-old Paint, Northstar. Assuming their daughter had already taken him out, he wasn’t too worried.
But once home, Jessie knew Loretta didn’t have Northstar. And it wasn’t like him to be off on his own. They immediately went looking. Jessie called. Hearing the voice he’d known since birth, Northstar whinnied. She called again. Loretta followed his whinnies to a swampy area. He was lying down, clearly in distress.
“His hide was all dirty and there were scratches on it,” said Woodworth. “I thought an animal had got hold of him. He got up and tried to follow me. I kept encouraging him and we managed to get him into the holding area.”

Northstar as a yearling. Photo: Jessie Woodworth
Very quickly the family realized their horse was in serious trouble. Northstar had been attacked, but not by an animal. To their horror, they realized that someone had entered the pasture, doused him in a flammable liquid and set him on fire.
Panic-stricken, he had raced away and rolled furiously, crushing small trees to put the flames out, scratching and tearing himself in the process. There were first, second, and third degree burns over 40 per cent of his body. The burns stretched from his neck, which had taken the brunt of the injury, across his shoulders where bone was exposed, and down his back.
The police were called and in the next few frantic days, Jessie worked with her vet to deal with Northstar’s wounds, dousing him with water, spreading soothing aloe on damaged skin, and adding electrolytes donated by a local feed store to his water. But his skin became so tight he could hardly walk. The Woodworths knew he needed far more help than they could give. Ten days after the original incident, they transported him to Ohio State University’s renowned Galbreath Equine Center.
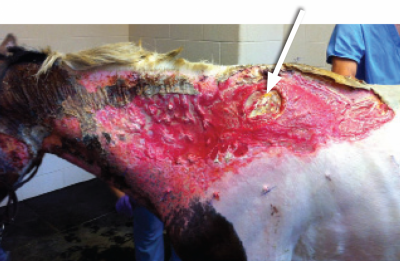
At day two in hospital, photo of Northstar’s left side shows that significant debridement has been performed. The arrow indicates the exposed scapula. Photo: Courtesy of Ohio State University
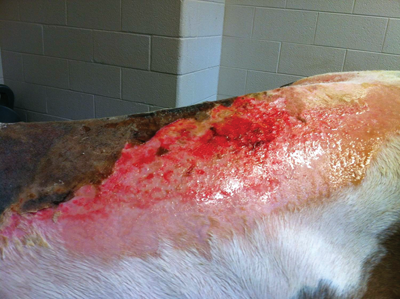
First and second degree burns down Northstar’s back. Photo: Courtesy of Ohio State University
“First was an assessment of his vital signs, respiratory effort, and establishment of IV access,” said Dr. Samuel Hurcombe, Assistant Professor in Equine Emergency and Critical Care. “We knew that his pain level was high, notably his first and second degree burns and that, at the very least, intravenous analgesia would be warranted. Because his neck was so damaged, I had to place an unusual type of catheter into his lateral thoracic vein on the side of his chest.”
Northstar was given morphine for pain, an anti-inflammatory, and a sedative. The wound was examined for severity, magnitude, and depth to assess what complications they were looking at in terms of long term survival.
Skin, the largest organ on the body, is made up of multiple layers of tissue that define the outer epidermis (the interface barrier with the environment) and the underlying dermis (that connects skin to tissue). It protects muscles, bones, ligaments, and internal organs, helps to regulate temperature, and guards against pathogens and water loss. Nerve endings provide sensations of heat, cold, touch, pressure, and pain. A first degree burn damages the epidermis; a second degree burn damages both the epidermis and the dermis; a third degree burn destroys all layers of skin to expose the tissue. All burns are intensely painful.
“There was debridement (dead skin removal) twice a day for the first two weeks,” said Hurcombe. “We cleansed his wounds to remove any pus (or) dead flesh, and promote a healthy healing bed of tissue. Debridement was both with bandage and gentle lavage, as well as surgically.”
Hurcombe used a saline solution as well as solutions to treat infection. Given the magnitude of Northstar’s injury, the veterinary team had to basically create a body wrap for bandaging. That proved to be especially hard when it came to keeping skin grafts in place.
Skin grafting involves slicing a piece of healthy skin from another area of the body with a tool called a dermatome. The harvested skin is placed on the cleaned, burned area with a bio-adhesive and kept in place with a snug bandage while it stabilizes. The donor site is dressed with a foam-type pad impregnated with silver which acts as an antibiotic, and then wrapped.
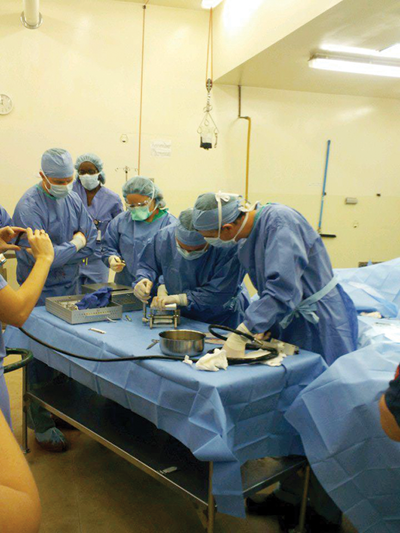
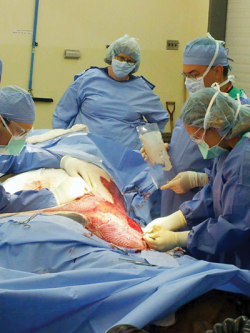
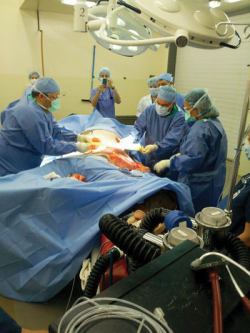
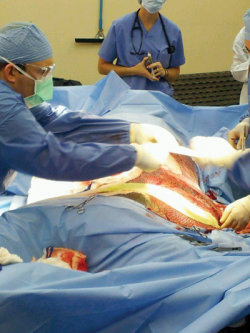
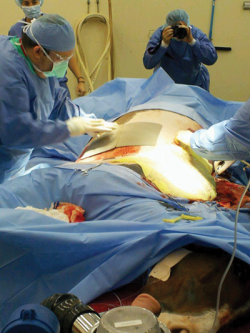
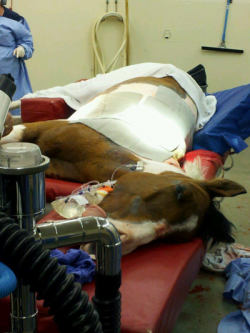
At Ohio State University’s renowned Galbreath Equine Center, equine surgeon Dr. Sanuel Hurcombe and human burn surgeon, Dr. Larry Jones, and their teams performed skin grafts to close Northstar’s wounds. Strips of graft skin were harvested from Northstar’s chest and belly, then put through a mesher to create tiny holes and expand the graft skin before applying it to the injured areas. As the graft took, the holes filled in with natural skin. One mesher surgery was done to cover the burned areas, along with numerous punch graft surgeries. Photos: Courtesy of Ohio State University
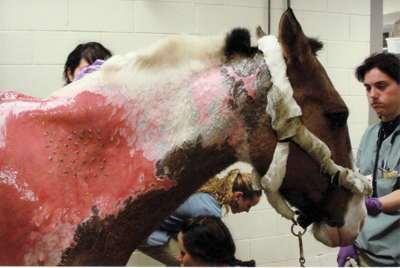
Dr. Holcombe tried several skin replacement strategies including punch grafts or pockets of skin taken from Northstar’s rump and planted in the neck and shoulder areas. Photo: Jessie Woodworth
Holcombe tried a host of different skin replacement strategies to close the wound and began with punch grafts by taking full skin thickness biopsies from the horse’s rump, creating little pockets in the burn wound, and “planting” them. They worked well over the shoulders and withers. But they were very small in a very large wound. So Hurcombe asked human burn surgeon Dr. Larry Jones, Associate Professor of Surgery and Clinical Director at Ohio State University’s Burn Center at the Wexner Medical Centre, for his help.
“The wound was very clean but I could see it needed a skin graft,” said Jones. “If we could do a mesher graft and expand it we would be able to cover a larger area with the graft. And it would get the wound closed a lot quicker than with punch grafts.”
Several strips of graft skin were harvested from the chest and belly. They were 10 centimetres wide, 23 to 25 centimetres long and 2 to 3 millimetres thick, twice the thickness that would be taken for a human. Sufficient skin was left at the donor site so that it could quickly heal. The strips were put through a mesher that cut tiny holes and expanded it to cover four times the area. At that stage, Hurcombe said, it looked like chicken fencing.
As the graft took, the holes filled in with natural skin growth. One mesher surgery was done to cover the burned area and several punch graft surgeries were done. But the complications of infection were ever-present. So was the challenge of dealing with severe itching, or pruritus, a tormenting side-effect as burned skin heals.
“Anti-inflammatories and medications for neuropathic pain were given (with) good results,” said Hurcombe. “It was important to minimize self-trauma of his healing wound and skin grafts. We had to put him on a wire (connected to the ceiling) to stop him lying down and traumatizing himself,” said Hurcombe, and added that Northstar also wore a neck cradle that made it impossible for him to bite his sides.
There was also the challenge of Northstar’s mental state. Burns are complex, deeply traumatic, long-term injuries. Having personally been burned by fire, I know that there is no pain like burn pain and with it come fear, anxiety, post-traumatic stress, frustration, and depression.

As burned skin heals, it becomes severely itchy. Dr. Hurcombe with Northstar wearing a neck cradle to keep him from biting his sides. Beyond the terror triggered by strangers, Northstar never lost his trust in people and those who loved him. Photo: Jessie Woodworth
“Mental stimulation, acceptance of care (and) being hospitalized for so long were challenging for him,” said Hurcombe. “We made every effort to spend time with him that was not always associated with a procedure, a needle etc. However, over time (several months), his attitude was harder to keep in good spirits. At that stage, I decided that pushing his treatment and grafting so hard was less important. He was stable, healing well, but I wanted his mental welfare to be better taken care of. After about four months, he went to a step-down facility that could take care of the day-to-day cleansing etc., but where he was able to see other healthy horses and not be in a hospital environment. He would come back for short periods of time for grafting and follow-up. Also, having frequent visits from the owner and other caregivers was so important. Getting outside, seeing the sunshine, making him feel like he was still a horse was our motivation.”
Nutrition is a huge part of healing burned patients and to his benefit Northstar never lost his voracious appetite.
“They need calories to heal,” said Jones. “Northstar was eating well and getting his nutrition. When he first came in and got over the deathly ill state, everyone was bringing him treats. He actually got fat.”
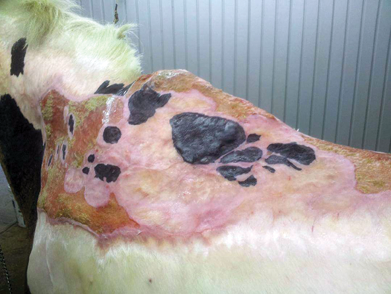
Northstar’s left side at approximately one year post-injury. Photo: Courtesy of Ohio State University
Northstar’s treatment has been unrelenting for 18 months. Infection was a constant threat. Preventing him from lying down and rolling required endless management and he had to overcome bouts of pneumonia. But his will to live never failed as healing progressed through the stages, and the grafts settled.
“Most are non-pigmented thin skin,” said Hurcombe. “There is some hair growing from the punch grafted areas where more of the dermal elements were included in the graft. (But) there will be significant scar tissue. The purpose of grafting is to limit this and thereby limit problems with range of motion, etc.”
The small sections of punch grafted skin were thicker when harvested and had more of the progenitor cells to support hair growth. How well the skin heals and thickens to become a permanent structure will determine whether Northstar can be ridden in the future with a perfectly fitted saddle and protective saddle pads.
“This will be looked into once he is completely healed and the new tissue is more mature,” said Hurcombe.
In addition to skin grafting, Northstar had cell therapy to promote skin growth.
“We essentially harvested his own dermal fibroblasts and keratinocytes,” he said. “We cultured them, then used his own plasma combined with bovine thrombin to make a ‘biological glue.’ (We) sprayed and injected the glue-cell mixture into the granulation bed.”
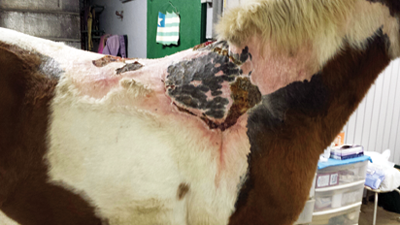
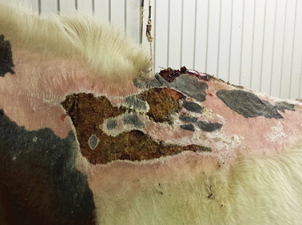
Photos taken in February 2014 show the dark blotchy area over the withers and shoulder where the punch grafts are growing and expanding, and hair is growing. Photos: Ruth Thompson-Carroll
Skin grafting and cell therapy have the same goal of regenerating skin. Hurcombe explained that grafting is like laying sod for immediate coverage and cell-based therapy is like planting seeds for growth and eventual coverage. This type of cell-based therapy had never been done in horses before but given that the cells were Northstar’s own, they expected – and got – good results.
“The cell therapy helped a lot,” said Jessie. “In combination with Ohio State and the vet we have now, he’s really come a long way.”
Hurcombe agrees. “Northstar is truly an amazing horse and despite having been viciously attacked by a human, he is still trusting. He has personality for sure, but, at the end of the day, it was his attitude and will to live that ultimately got the team of people together to heal this horse. Euthanasia was discussed right at the beginning and especially during the first month. Having never treated a case like this, we weren’t exactly sure that we could. From humane grounds, euthanasia was a real and valid option, but with endless emotional (and financial) backing and support, we at OSU were willing to do whatever we could to give this horse another chance at life as long as he was willing to fight.”
The American Association of Equine Practitioners sets five criteria as guidelines to help make a humane decision about euthanasia. They are:
- A horse should not have to endure continuous or unmanageable pain from a condition that is chronic and incurable;
- It should not undergo a medical or surgical condition with a hopeless chance of survival;
- It should not be kept alive if it has an unmanageable condition that makes it a hazard to itself or its handlers;
- It should not have to receive continuous analgesic medication for pain relief for the rest of its life; and,
- A horse should not have to endure a lifetime of continuous individual box stall confinement for prevention of unmanageable pain or suffering.
As dire as Northstar’s initial condition was, he did not meet any of those criteria.
The cost to save Northstar’s life ran into six figures and an anonymous donor stepped forward to pay expenses. Despite the police investigation, no one has yet been arrested for the crime and it remains an open case.
For everyone whose lives have been touched by Northstar, they not only see an amazing horse but greater insights in themselves.
“The day we did the first surgery I took my whole team,” said Jones. “Dr. Hurcombe has quite a team and it was really neat to see the two teams come together and recognize there were more similarities in their work than differences as they applied their knowledge in their respective fields. We all wanted this animal to do well. A lot of people cared for him.”
None more than the Woodworths, who kept vigil in Pennsylvania and agonized over the intense cruelty inflicted on the horse they cherished and had raised from birth. But through the ordeal came new strengths.
“You see how strong family bonds are and how many horse lovers there are out there,” said Jessie.
It haunts her that perhaps two people were involved – one holding Northstar (he had no halter on) and another dousing him with the liquid. Yet beyond the terror triggered by strangers, Northstar never lost his trust in people and those who loved him.
“He waited for us,” said Jessie softly, recalling that awful day. “He had willpower. My vet said to give him a chance but we didn’t know what Ohio State would say. They don’t want to give false hope or struggle if a horse won’t make it. If I’d had to euthanize Northstar I would have done it.”
Today Northstar enjoys life with other horses in a secured location in Pennsylvania. He is 90 per cent healed and is allowed to graze, even roll a little, and loves to be lunged.
“He always had that look in his eye that said ‘I’m still here,’” said Jessie. “God kept him around. I don’t know the reason yet. I still have faith I’ll get on his back again someday.”
“Until he extends his circle of compassion to all living things, man himself will not find peace.” – Albert Schweitzer
Main photo: Dr. Vikki Scottand Dr. Samuel Hurcombe with Northstar. “It was his attitude and will to live that ultimately got the team of people together to heal this horse.” – Dr. Hurcombe. Courtesy of Ohio State University